One Health Newsletter
COVID-19 Epidemic Brings Black Fungus into the Limelight in India
Authors
Rishendra Verma
Emeritus Professor
Indian Council of Agricultural Research
Indian Veterinary Research Institute
Izatnagar, India
Introduction
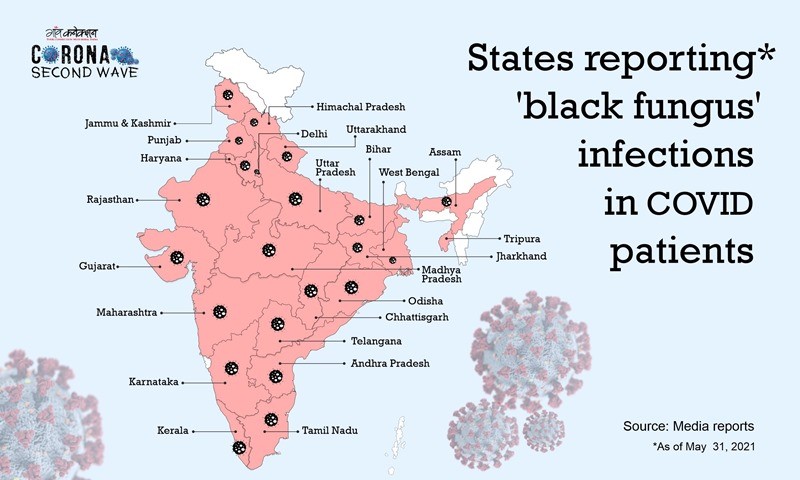
Lurking in the background of the Indian COVID-19 epidemic, black fungus infections (mucormycosis, phycomycosis or zygomycosis) have been on an unexpected rise, leading the Government of India to use One Health joint efforts to address such a fungal scourge. Since 2019, at the inception of COVID-19 in India, more than 8,800 cases of black fungus have been reported in India. Five states of India, Tamil Nadu, Odisha, Gujarat, Rajasthan, and Telangana, have declared black fungus as a notifiable disease under the Epidemic Diseases Act, 1897.1 In addition, cases of black fungus have been reported in other Indian states, including Maharshtra (1,500), Gujarat (1,163), Madhya Pradesh (575), Haryana (268), Dehli (203), Uttar Prdeash (169), Bihar (103), Chattisgarh (101), and Karnataka (97) (Figure 1).2
Figure 1: The map shows cases of black fungus in various States of India
Source: GaonConnection, 6 July 2021
According to the Indian Council of Medical Research (ICMR)4, the following conditions in COVID-19 infected patients increases the risk of developing a mucormycosis infection: uncontrolled diabetes, weakened immune system (steroid use, organ transplant or cancer) prolonged intensive care unit or hospital stays, and voriconazole therapy (i.e., treatment of invasive fungal infection). These observations were disseminated after previous epidemiological reports of mucormycosis infection were documented, where 83 out of 100 COVID-19 positive cases suffered from diabetes, 45 out of 45 COVID-19 positive cases had diabetes, and two paediatric COVID-19 positive cases were diabetic, noting that diabetes weakens immunity and increases susceptibility of COVID-19 infection.5
In a recent study (2019-2020), the prevalence of mucromycosis was reported to be nearly 80 times higher in India than in developed countries.3 The article aimed to provide glance in light of the status of black fungus and its link with COVID-19 patients as well as the magnitude of problem in India. The efforts made by Indian veterinary and medical experts, doctors, and government are presented in this article.
Black Fungus Characteristics and Treatment
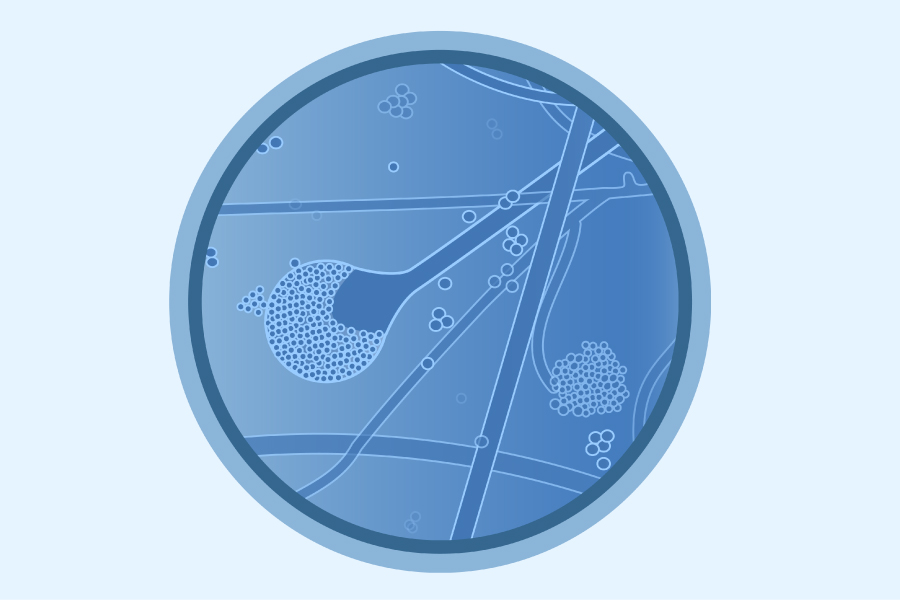
Black fungus infection or mucormycosis is an opportunistic fungal infection that interrupts the blood supply to normal tissue that becomes black due to necrosis, hence the name "black fungus". Mucormycosis occurs in humans as well in domestic and wild animals (cattle, sheep, cats, dogs, cows, horses, dolphin, bison, and seals). The types of opportunistic fungi that cause mucormycosis include several species that are found worldwide: Mucor irregularis, Rhizopus homothallicus, Syncephal astrum, Cunninghamella bertholletiae, Apophysomyces variabilis, and Litchthemia spp. (formerly called Absidia). Rhizopus oryzae, R. micosporous, and Apophysomyces variabilis have been reported in India. R. oryzae (Figure 2), the most common type of black fungus, is responsible for nearly 60% of mucormycosis cases in humans and accounts for 90% of the rhino-orbital-cerebral (ROCM) form in India.6 Mucormycosis may be gastrointestinal (swallowed fungal spores), cutaneous (when fungus enters through a break in skin), or disseminated in form (when the infection spreads through the bloodstream, affecting other organs in the body). This fungus can cause pain, redness around eyes and/or nose, fever, headache, shortness of breath, coughing, and vomiting blood. Lung or sinus infections sometime requires major surgery to remove the eye or part of diseased skull and jaw.
Figure 2: Mucormycetes (Source: CDC, 2021: https://www.cdc.gov/fungal/diseases/mucormycosis/causes.html).
Black Fungus and COVID-19
The possibility of heavy contamination in medical oxygen cylinder pipes and hospital humidifiers cannot be ruled out during prolonged hospitalization of COVID-19 patients. Airborne fungal spores are the major source of hospital indoor contamination, which increases the risk to COVID-19 patients acquiring an airborne nosocomial infection. Due to the shortage of beds, oxygen supply, and ventilators, COVID-19 patients can become frantic to seek hospitalization. In certain situations during the sudden demand of ventilators and medical oxygen supply, the air ways of ventilators may become exposed to humidity in the rush to aid patients, facilitating fungal infection. Monitoring of Indian hospitals for the presence of fungi is not generally undertaken; rather, the emphasis is on sanitization of the premises. This is a realistic concern, since a previous study revealed that airborne fungal monitoring of 160 samples collected from different wards and operating rooms in India yielded 7 genera of fungi.7
The ICMR4 has issued an advisory on the diagnosis and treatment of black fungus. Amphotericin B is considered the drug of choice for the treatment of black fungus. This drug selectively inhibits the synthesis of ergosterol, a sterol unique to fungal cell membranes, causing the formation of pores that cause rapid leakage of contents, followed by fungal cell death. The Indian government granted approval to produce more injections by more pharmaceutical firms to meet increased demand.
Moving Forward
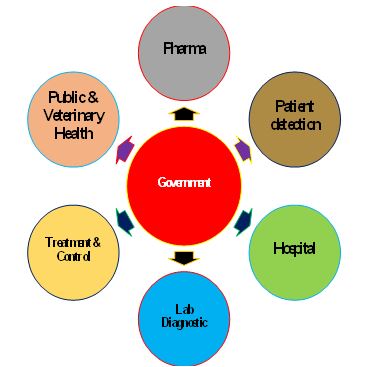
Figure 3: Model diagram showing how the Indian government is involved in bringing One Health aspects together to combat black fungus infections.
For the first time in India, veterinary research laboratories are actively working with medical doctors in collective response efforts, recognized as the most significant One Health activity in the country with the support of the government (Figure 3). They are jointly diagnosing COVID-19 by RT-PCR and promoting regular surveillance and stringent measures for disease control. These approaches include air disinfection systems, ventilation systems, the use of high-efficiency particulate air (HEPA) filters for high-risk wards, closing the windows, control of entry and exit doors, and the control or complete elimination of flowers brought into hospitals by patient visitors that are necessary to reduce fungal spores in the environment.8 Patients infected with COVID-19 and black fungus calls for joint efforts of veterinarians and medical experts under the umbrella of One Health for rendering prompt diagnosis, treatment, and prevention. The need of utilizing the skills of veterinarians arose due to their competence in the RT-PCR laboratory in the wake of the emergent situation needing prompt diagnosis of COVID-19 in human samples. In the interest of time, veterinarians and medical experts were required to share responsibilities and actions under the One Health umbrella in order to better manage the black fungus and COVID-19 outbreaks.
Hopefully, the lessons learned in this pandemic will prepare India to meet future health challenges, including collaborative support between veterinary and human medicine professionals. The policy makers and administrators responsible for decision making in government of India have realized that teamwork utilizing a One Health approach is one of the most valuable lessons learned from the COVID-19 pandemic.
References
- Hindustan Times. These states have declared 'black fungus' a notifiable disease. https://www.hindustantimes.com/india-news/these-states-have-declared-black-fungus-a-notifiable-disease-101621565107184.html. Updated on May 21, 2021. Accessed on June 14, 2021.
- Hindustan Times. Black fungus: Here is a list of states with highest number of mucormycosiscases. https://www.hindustantimes.com/india-news/black-fungus-states-with-highest-number-of-mucormycosis-cases-101621559394002.html. Updated on May 21, 2021. Accessed June 14, 2021.
- Singh AK, Singh, R, Joshi SR, Misra A. Mucromycosis in COVID-19: A systematic review of cases reported worldwide and India. Diabetes Metab Synd. 2021;15(4):102146.
- Press Information Bureau of the Government of India. Stay safe from Mucormycosis - a fungal complication being detected in COVID-19 patients control diabetes, use steroids judiciously, keep good hygiene, don’t self-medicate. https://pib.gov.in/PressReleseDetailm.aspx?PRID=1718501. Updated May 14, 2021. Accessed June 14, 2021.
- British Broadcasting Company News. Black fungus: India reports nearly 9,000 cases of rare infection. https://www.bbc.com/news/world-asia-india-57217246. Updated on May 23, 2021. Accessed June 14, 2021.
- Prakash H, Chakrabarti A. Global Epidemiology of Mucormycosis. J Fungi (Basel). 2019;5(1):26.
- Shashi C, Mahajan G, Singh Y. Monitoring of airborne fungi in a hospital unit. IJCP. 2000;31(1):20-23.
- Arunaloke C, Sekhar CS, Shivaprakash Overview of opportunistic fungal infections in India. Nihon Ishinkin Gakkai Zasshi. 2008;49:165.
One Health Newsletter
The One Health Newsletter is a collaborative effort by a diverse group of scientists and health professionals committed to promoting One Health. This newsletter was created to lend support to the One Health Initiative and is dedicated to enhancing the integration of animal, human, and environmental health for the benefit of all by demonstrating One Health in practice.
To submit comments or future article suggestions, please contact any of the editorial board members.